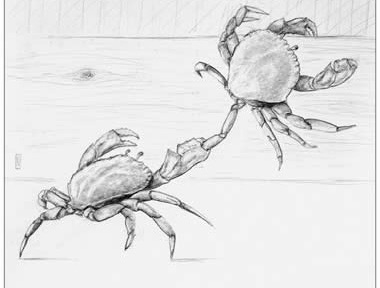
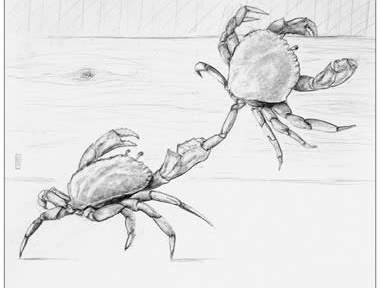
Crabs in a bucket: Marvin (Diné / Navajo) reflected on “Crabs in a Bucket.” An elder in Seattle shared commonly told admonishment that crabs pull each other down, if one tries to climb out of a pot or bucket, other crabs pull it back down. The lesson, be cautious of who is around you.
In nature, however, Crabs actually cooperate, climb on each other, help each other, live in community in order to survive. Their nature is cooperation. The bucket, the elder said, is a Western construct. The bucket is Western society, materialism, individuality. When pulled away from their natural environment, of course crabs behave differently.
A beautiful Native-American re-interpretation of a story commonly told to children; don’t trust or be pulled down by those around you. This stands is stark contrast to Crabs’ true nature, to lift each other up.
Adam Grant (Wharton) added, “We assume this is how crabs behave in a bucket bc this is what we’ve been told. Researchers showed, however, they don’t actually pull each other down. ….Test the hypothesis.”
Native wisdom.
 “Jamés, is there any chance you can take tomorrow off? Do you want to go mountain bike riding in the rain 🌧️ ☔️ ?? It’s really beautiful, and there’s place in Marin where it’s not muddy and we can have a beautiful ride. China Camp in Marin.”
“Jamés, is there any chance you can take tomorrow off? Do you want to go mountain bike riding in the rain 🌧️ ☔️ ?? It’s really beautiful, and there’s place in Marin where it’s not muddy and we can have a beautiful ride. China Camp in Marin.”

